![]()
DERMATOLOGY FOR ADULT PRIMARY CARE (KP) * Derm Cortisone Drugs | Topical_steroids2009.pdf
http://www.modernmedicine.com/dermcounselor
What To Look For: The ABCD's of Moles and Melanoma
REF: Dr. Arndt's Dermatology in Primary Care 2002 Kenneth Arndt, MD
Scaling & Proliferative Skin Disorders:
Acne & Related Skin Syndromes
Infestation: Lice (Pediculosis) & Scabies
Precancerous Growths & Skin Cancer:
Primary Lesions
Macules: Circumscribed flat discolorations of the skin; less than
1 cm in diameter.
Examples: freckles, flat nevi
Patches: Circumscribed, flat discolorations of the skin greater than
1 cm in diameter.
Examples: vitiligo, solar lentigines
Papules: Circumscribed, superficial, elevated, firm lesion less than
1 cm in diameter.
Examples: elevated nevi, warts, lichen planus
Plaques: Circumscribed, elevated, superficial, firm, rough lesions with a flat top surface greater than 1 cm in diameter. Examples: psoriasis, mycosis fungoides
Wheals: Elevated irregular-shaped areas of cutaneous edema; transient,
with variable diameters.
Examples: hives, insect bites
Nodules: Solid lesions with depth; they may be above, level with or beneath the skin, 1-2 cm in diameter. Examples: nodular basal cell carcinomas, xanthomas
Tumors: Solid lesions; may or may not be clearly demarcated; they may be above, level with or beneath the skin surface; greater than 2 cm in diameter. Examples: neurofibromas, large basal cell carcinomas and xanthomas
Vesicles: Circumscribed, superficial elevations of the skin containing serous fluid; less than 1 cm in diameter. Examples: herpes simplex, herpes zoster, contact dermatitis
Bullae: Circumscribed, superficial elevations of the skin containing serous fluid; greater than 1 cm in diameter. Examples: pemphigus vulgaris, bullous pemphigoid, second-degree burns
Pustules: Circumscribed elevations of the skin containing purulent fluid. Examples: acne, impetigo
Cysts: Elevated, circumscribed, encapsulated lesions; in dermis or subcutaneous layer; filled with liquid or semi-solid material. Examples: acne, epidermal inclusion cysts
Petechiae: Small (up to 4 mm), circumscribed, non-palpable deposits of blood or blood pigments.
Purpura: Larger (greater than 4 mm), circumscribed deposits of blood or blood products in the skin. Example: bruises
Secondary Lesions
Scales: Shedding, dead epithelial cells that may be dry or greasy.
Examples: dandruff, psoriasis
Crusts: Dried serum, blood, or purulence. Examples: impetigo, infected dermatitis
Excoriation: Abrasions of the skin resulting in loss of epidermis; usually superficial and traumatic. Examples: scratched insect bites, scabies
Fissure: Linear crack or break in the epidermis; may be moist or dry
Lichenification: Diffuse area of thickened epidermis secondary to persistent rubbing, itching, or skin irritation with resultant increase in the skin lines and markings; often involves flexor surface of extremities. Example: atopic ermatitis
Scar: Thin to thick fibrous connective tissue that replaces normal skin following injury or disease.
Keloid: Irregularly shaped, elevated, progressively enlarging scar; grows beyond the boundaries of the wound; caused by excessive collagen formation during healing.
Erosion: Loss of part of the epidermis or mucosa; depressed, moist, glistening; follows rupture of a vesicle or bulla.
Ulcer: Loss of epidermis and dermis; concave; vary in size; often
with moist or crusted material.
Examples: Can occur within areas of stasis dermatitis of the legs
Atrophy: Thinning of the skin surface and loss of skin markings; skin translucent and paper-like.
Special Lesions and Descriptive Terms
Burrows: Small and short or long and tortuous tunnels in the epidermis. Examples: small and short burrows (scabies); long and tortuous burrows (creeping eruptions)
Comedones (Blackheads): Plugs of whitish or blackish sebaceous and keratinous material lodged in the pilosebaceous follicle usually seen on the face, the chest and/or back. Example: acne
Milia (Whiteheads): Whitish papules, 1-2 mm in diameter with no visible opening onto the skin surface. Examples: healed burns, healed bullous disease states, face of newborn babies
Telangiectasias: Dilated superficial blood vessels that appear as fine irregular red lines. Example: spider angiomas
Eczematous: This term is used to describe inflammatory conditions of the skin, which appear erythematous and scaly with ill-defined borders. Examples: atopic dermatitis, irritant dermatitis, tinea.
Papulosquamous: This term is used to describe conditions, which manifest themselves as papules or plaques with scales. Examples: psoriasis, lichen planus, pityriasis
Necrosis: Death of skin that appears black or dark green or purple in color.
Wet/Oozing: The water barrier of the skin has been damaged and there is enough flow of fluid from below to keep the surface of the lesion wet.
When referring:
Please specify duration, location, morphology, any treatments already tried, and the patient's current medications. Please instruct the patient to bring all oral and topical prescriptions and OTC medications they are currently using.
Dermatologic Conditions Commonly Seen in Adult Primary Care
See also
Acne page
ACP PIERS http://pier.acponline.org/physicians/diseases/d613/d613.html)
Clogged pores and a reaction to the bacterium Propionibacterium (P. acnes) cause acne. It is characterized by comedones, blackheads, whiteheads, papules, pustules , nodules, cysts, & scars on the face and/or trunk. Almost all teenagers and many younger adult women have acne. In young adult women, the lesions often occur about the mouth and along the jaw-line and chin.
Classification of Acne -
Its
Severity & Types (ACP PIER)
Drug Treatment for Acne -
http://pier.acponline.org/physicians/diseases/d613/tables/d613-tdtx.html
Therapy of Acne
Mild: topical - benzoyl peroxide, tretinoin, adapalene (Differin)
Moderate: add oral antibiotics as tetracycline, doxycycline, erythromycin
Severe: minocycline, isotretinoin (Accutane).
50% of people after a course of Accutane usually stay clear indefinitely,
and of the other 50%, 10 or 15 may require a second course at some point,
and the others have some disease, usually less than before
For mild acne, select an appropriate topical
regimen.
Specific recommendation:
Before selecting topical therapy, consider the patient's skin type:
Dry, Sensitive, Combination (having both oily and dry areas), Normal, Oily
For dry and sensitive skin types, avoid:
High concentrations of benzoyl peroxide (5%)
Strong topical retinoids (standard tretinoin gel and tazarotene gel)
Irritating vehicles (hydroalcoholic gels and solutions)
When mild acne is mainly noninflammatory (comedonal),
treat with a topical comedolytic agent, particularly a retinoid (tretinoin, adapalene, or tazarotene).
For patients with known retinoid intolerance,
consider benzoyl peroxide, azelaic acid, or a keratolytic agent.
When mild acne is mainly inflammatory (papulopustular), add a topical antibacterial agent to a comedolytic agent:
In the morning, use a topical benzoyl peroxide, erythromycin, clindamycin, or a fixed-combination antibacterial product
At bedtime, use a topical retinoid
Agents effective for Comedones: Retinoids, azetaic acid, salicyclic acid
Agents effective for inflammatory lesions: benzoyl peroxide, tretinoin, azetaic acid, topical erythromycin & clindamycin, Na sulfacetamine
Recommendations Regarding Oral Antibiotic Use in Acne:
Oral antibiotics as: Tetracycline, Doxycyline, Erythromycin, Minocycline, trimethoprim & Sulfamethoxazole (Septra or Bactrim DS), Clindamycin should not be used when topical preparations will suffice
Continue antibiotic Rx for no longer than is necessary (usually may be over 6-8 weeks)
If further Rx is required after an antibioc has been discontinued, reuse the original antibiotic whenever possible
Avoid concomitant oral & topical therapy with chemically dissimilar antibiotics to reduce the risk of developing resistance to both
Treatment
Wash face twice a day with mild cleanser.
Use only non-comedogenic products on the face. Use moisturizer with sunblock.
Antimicrobials kill the bacteria. Common antimicrobials include benzoyl peroxide and topical antibiotics.
Retinoids help to open the pores. Retinoids include Tretinoin (Avita® 0.025% or Retin A® Cream) and Adapalene (Differin® Gel).
Mild acne: (Primarily blackheads):
Excellent topical therapy combines topical retinoids e.g. Tretinoin (Avita® 0.025% cream, Retin A®) or Adapalene (Differin® gel) 45 grams QHS and over-the-counter benzoyl peroxide 5% QAM. Note: Benzoyl peroxide may bleach clothing. If too irritating, try Sulfur and Sodium Sulfacetamide (Novacet®, Sulfacet®), or Clindamycin (Cleocin T®) topical solution. Give any topical therapy at least 6 weeks to assess effectiveness. For mild acne, topical therapy over 6 weeks is usually very effective. The patient must apply topical medications all over. For acne on chest, shoulders, and back: Apply benzoyl peroxide 10% QHS. No spot treating.
Moderate Acne: (Papules, pustules, or unresponsive to the above treatment)
If the acne is not responsive or there is moderate, inflammatory facial acne, add Tetracycline 500 mg BID or Doxycycline (Vibramycin®) 100 mg BID. Caution patient about sun exposure. Give any regimen 6 weeks. If the acne fails to respond, refer to Dermatology.
Severe Acne: (Numerous cysts, scarring,
or unresponsive to the above treatment)
If scarring is occurring, therapy must be aggressive.
Refer directly to Dermatology.
Oral retinoid therapy, e.g. Isotretinoin (Accutane®), is often recommended for treatment of severe recalcitrant acne.
During pregnancy: Therapy is limited to topical benzoyl peroxide and erythromycin. In unusually severe cases, consult with OB/GYN to consider oral erythromycin.
Acne Keloidalis
Rx: (Dr. S.Y.)
ACNE ROSACEA (SEE ROSACEA)
Actinic keratoses are sun-induced precancerous lesions. They present as persistent, scaly, red lesions and are often better felt than seen. Patients often say the spots hurt or sting.
Look and feel for actinic keratoses in the chronically sun exposed areas,
e.g. nose, forehead, temples, sides of cheeks, ears, back of the hands, arms,
etc.
Cumulative photodamage to ultraviolet UVB
Enlarge in summer, regress in winter
Precancerous: may progress to Squamous Cell Cancer & cause metastatic to nodes in 2-6%.
Treatment
Cryosurgery: liquid nitrogen
Electrosurgery & curettage
Mild acids: trichloroacetic acid TCA
Topical chemotherapy: Efudex, 5% 5-fluorouracil (5-FU) bid for 2-4 wks
Carbon dioxide laser for cheilitis
Sunscreens
Refer patients presenting with greater than 15 lesions, with lesions on mucous membranes, and/or lesions failing to respond to recommended liquid nitrogen therapy.
Apply liquid nitrogen once to an actinic keratosis. Lesion should be sprayed until it turns white with a 1 mm margin. The treated lesion should stay white (frozen) for only 10-15 seconds. Longer freezing may result in ulceration. Discuss risk of blister and white discoloration that result from cryotherapy. Advise patients that they may need to be examined and treated annually for actinic keratoses.
Recommend DAILY MORNING SUNSCREEN (at least SPF 15 or SPF 30 or higher).
ALOPECIA AREATA (See Hair Loss.)
Frequently flexural. Asthma and allergic rhinitis are often associated. Thickening of the skin (lichenification) indicates chronic scratching. Crusting may indicate Herpes or Staph infection.
Treatment
Advise patient to shower or bathe once daily for 5 minutes in cool to warm (not hot) water. Use mild, non-perfumed, non-dyed cleansers (e.g. Dove® unscented, Cetaphil®, Aquanil®, Purpose®, Aveeno®, Basis®). Apply a moisturizer (Cetaphil®, Eucerin®, Aquaphor®, SBR-Lipocream® or Vaseline®). No lotions please as they are more drying!
Apply topical steroids immediately after the bath/shower while still "sticky". May use Triamcinolone acetonide (Kenalog®) 0.025% or 0.1% ointment for teenagers and young adults. Avoid higher potency topical steroids on the face and body folds. Use Class VI or Class VII steroids in these areas. (See Table 1.)
Consider oral antihistamines Diphenhydramine or Hydroxyzine (Benadryl® or Atarax®) if scratching is a large component of the disease. They make the patient drowsy and less likely to scratch.
Have the patient use the topical steroid as needed, for flares and for stubborn areas. Cephalexin (Keflex®) or Dicloxacillin (Dynapen®) 500 mg QID for 10 days may be helpful if secondarily infected or treatment-resistant. Control but not cure is expected. Make sure it is eczema and not tinea as topical steroids may cause fungus to flourish.
Instruct patients that humidifiers are helpful in dry environments. Avoiding dust, wool, and animal dander may be helpful. Rarely does food play a role in atopic dermatitis. If food allergies are suspected, refer patient to allergy.
See dry skin treatment guidelines which may be helpful in treating atopic dermatitis.
BACTERIAL INFECTIONS
(Impetigo, Folliculitis, Cellulitis)
![]()
![]()
See Cellulitis, etc. - Johns Hopkins Advanced Studies in Medicine Feb 2006
Common bacterial infections affecting the skin include impetigo, folliculitis, and cellulitis.
Impetigo
Impetigo is a common, contagious, superficial skin infection that is produced
by streptococci, staphylococcus, or a combination of both bacteria. It can
be vesicular/bullous or non-vesicular/non-bullous. It is characterized by
honey-colored crust.
Treatment
For widespread involvement: Use an oral antibiotic such as Dicloxacillin (Dynapen®) or Cephalexin (Keflex®) 250-500 mg for 5-10 days.
For localized involvement: Use Mupirocin (Bactroban®) ointment three times/day until all lesions have cleared.
Culture areas of recurrent impetigo.
Folliculitis
Images
of Folliculitis
Images
of Furuncle
Staphylococcal folliculitis is the most common form of infectious folliculitis.
Folliculitis usually appears as multiple pustules with surrounding erythema.
Treatment
Use oral antibiotics, e.g. Miinocin 100 mg bid, Dicloxacillin (Dynapen®), Cephalexin (Keflex) 250-500 mg QID for at least 2 weeks.
Topical Bactroban ointment 2-3x/day
Topical soothing Pramosone lotion bid if needed for burning itching and pain
Cellulitis
An infection of the dermis and subcutaneous tissue usually caused by Group
A Streptococci and Staph aureus in adults. Typically occurs near surgical
wounds or a cutaneous ulcer but may develop in apparently normal skin. Recurrent
episodes occur with local anatomic abnormalities. Erythema, warmth, edema
and pain are all distinctive clinical features.
Treatment
Antibiotics against MRS, such as SeptraDS/BactrimDS
(trimethoprim-sulfamethoxazole) and Clindamycin are more effective and preferred
empiric therapy than Cephalexin for outpatients with cellulitis in the
community-associated MRSA-prevalent setting.
(REF: AMJ Oct 2010; 123, 942-950 Thana Khawcharoenporn, Alan Tice,
MD)
Treat appropriate adults empirically with anti-staph and anti-strep antibiotics e.g. Dicloxacillin (Dynapen®)) 500 mg QID or Erythromycin or a Cephalosporin (Keflex™) 250-500 mg QID.
BENIGN SKIN CONDITIONS (Cosmetic- See Appendix A.)
CELLULITIS (See Bacterial Infections.)
Lesions are microvesicular or eczematous.
Look for linear or bizarre shaped lesions.
Treatment
Advise patient to wash all objects that have come in contact with the allergen. Avoid topical benadryl and "caine" related products. Twice daily warm soaks may be applied to crusted, oozing areas.
For widespread involvement:
Use Prednisone. Recommended treatment includes a systemic prednisone burst
of 0.75 mg/kg/day for 5-7 days followed by a tapering course of prednisone
over the next 10-14 days. Avoid Medrol® dose pack alone as it uses inadequate
dosing. It may, however, be used in conjunction with IM Kenalog®. Use
a topical steroid cream or ointment as well, e.g. Betamethasone Valerate
(Valisone®) 0.1% BID until clear.
For limited involvement:
Use Betamethasone Diproprionate (Diprolene®) 0.05% ointment or Clobetasol
(Temovate®) ointment BID for 2-3 weeks.
For allergic contact dermatitis of the face:
Use either prednisone as outlined above or Betamethasone Valerate
(Valisone®) 0.1% cream BID for 7 days, then Desonide (Desowen®) 0.05%
cream or another less potent steroid until rash is clear.
Benadryl® or Atarax® may be helpful for nighttime itching.
Dry skin itches! Treat the dry skin and the itch will go away. If there is redness, xerotic eczema may have set in.
Treatment
For dry skin:
Use Eucerin® or Cetaphil ® cream, Aquaphor®, Vaseline® or
SBR-Lipocream® applied to affected skin immediately after the bath/shower.
Ointments are better than creams. Lotions are less effective.
For more scaly skin:
Consider the use of OTC medicated products (e.g. Amlactin Lotion®, Eucerin
Plus™, Lubriderm®, Carmol® 10%).
For xerotic eczema:
Treat dry skin as above and add a topical steroid e.g. Triamcinolone acetonide
(Kenalog®) 0.1% ointment.
DYSHIDROSIS (See Hand
and Foot Eczema.)
![]()
![]()
FOLLICULITIS (See Bacterial Infections.)
FUNGUS (See Tinea Infections.)
HAIR LOSS (Alopecia)
![]()
![]() See also
Alopecia (Hair Loss)
See also
Alopecia (Hair Loss)
REF: Cleveland Clinic J of Med August 2003 Alopecia
If you suspect an underlying disease, order the following labs: TSH, CBC, and Ferritin (should be above 40). If there are signs of virilization (irregular menses, hirsuitism, change in body habitus, deepening voice and/or severe acne), consider ordering: Total Testosterone and DHEAS.
If all normal or negative, diagnosis is androgenetic alopecia
Androgenetic Alopecia
Hair loss in men and women is usually androgenetic alopecia. Treatment is not a covered benefit. Be very sensitive as both men and women are often very psychologically bothered by hair loss.
Look for the pattern of hair loss. Hair loss on the top of the scalp is usually androgenetic. Another useful clue can be to identify whether hair is falling out from the roots or breaking off. A family history of hair loss is NOT that reliable. Hair breakage is often caused by treatments to the hair. Can suggest that patient try Rogaine 2-3% (OTC) or 5% (Rx) topically BID. Women can only use 2% Rogaine.
Telogen Effluvium
New onset of diffuse hair loss called telogen effluvium can be caused by acute stress to the body. This occurs about 100 days after a stress such as pregnancy, severe illness or surgery, drugs (e.g., Beta-blockers, warfarin, Depo-Provera®) and abnormal diets (crash diets, excess Vitamin A). Make sure scalp is normal and that hair is falling out from root, not breaking.
Alopecia Areata
Appears as smooth, round areas of hair loss. Is commonly caused by stress and may be associated with thyroid disease.
Treatment
For alopecia areata: Consider initiating twice daily topical steroid therapy, e.g. Betamethasone Diproprionate (Diprolene® augmented gel) 0.05% and refer to Dermatology.
HAND AND FOOT ECZEMA (DYSHIDROSIS)
![]()
![]()
Very common. Typical clinical features include red, scaly fissuring, small vesicles. Other things to consider in the differential diagnosis include irritant contact dermatitis and scabies, especially if there is web-space involvement with blisters and burrows. If the nails are dystrophic, consider tinea (two-foot, one-hand disease).
Treatment
Identify and advise the patient to avoid triggers. Otherwise, advise the use of gloves any time hands are in water, e.g. washing dishes and cleaning. Apply a heavy cream (e.g. Eucerin® cream or Neutrogena® hand cream) to hands multiple times per day, especially after hands have been wet and Betamethasone Diproprionate (Diprosone®) 0.05% ointment BID for redness. For painful fissures, antibiotic ointment (e.g. Bacitracin® or Poysporin®) ointment covered by bandage. Avoid Neosporin®) as neomycin is a common sensitizer! If these treatments fail, add Cephalexin (Keflex®) 250 mg QID for 10 days. If no improvement despite these measures, refer to Dermatology.
Herpes simplex is a virus that can infect any part of the skin, lips, or genitalia. The most common location for a flare of herpes is the border of the lip ("Cold Sore", "Fever Blister"). Colds, fever, and sun exposure are frequent triggers. Initially the patient may feel tingling, burning, or pain in the affected area. Within a day or so, the skin becomes swollen and red. Individual vesicles may be seen. Crusting follows after several days.
Herpes simplex may also occur on the finger (Herpetic Whitlow). This is a common presentation in people who often have their hands in patient's mouths, e.g. dentists or their assistants.
Herpes genitalis classically appears as grouped vesicles on an erythematous base; however, this is not frequently seen. Instead, localized pain, erosions, or erythema may be all that is seen.
Herpes simplex often develops on the buttocks of women. Why this occurs is unknown.
Treatment
For primary infections: Acyclovir (Zovirax®) 200 mg capsules 5 times/day for 10 days or 400 mg tablets 3 times/day for 10 days
For recurrent infections: Acyclovir (Zovirax®) 200 mg 5 times/day for 5 days or 800 mg twice daily for 5 days. Treatment should be initiated at the earliest sign of symptoms (prodrome) or recurrence.
For chronic suppressive therapy: Acyclovir (Zovirax®) 400 mg 2 times/day for 6-12 months.
Patients should be told that the condition is contagious and spread by contact.
HERPES ZOSTER (SHINGLES)
in a normal host
![]()
![]()
See also Shingles (Herpes Zoster) | Postherpetic-Neuralgia
Herpes Zoster presents as groupings of vesicles on an erythematous base. There may be multiple groupings in one dermatome. Pain may be significant and frequently precedes the onset of the rash.
Treatment
Acyclovir (Zovirax®): Start therapy within 72 hours after the onset of the rash; best results are seen when therapy is initiated 48 hours after the onset of the rash; no significant reduction is seen if therapy is initiated 72 hours after onset. Give 800 mg 5 times/day for 10 days (every 4 hours while awake).
Burow's Solution® or cool tap water in wet compresses can be applied to weepy areas BID-TID to dry them out.
Provide adequate pain management. Do not give systemic steroids.
If the patient presents with eye symptoms, refer to Ophthalmology.
Hidradenitis Suppurativa is a chronic disease of the regions of apocrine gland activity. It begins as firm, tender, red nodules and develops into large sinuses under the surface of the skin. These sinuses drain pus and whereas some of the first lesions heal quickly, new nodules continue to form. Mostly seen on the groin, axillae, buttocks and the breasts, it is most common in young women. Many cases, especially of the thighs and vulva, are mild and misdiagnosed as recurrent furunculosis. The disease is worse in the obese. Click on Image to zoom.
A hallmark of hidradenitis is the double comedone, a blackhead with two or sometimes several surface openings that communicate under the skin. This distinctive lesion may be present for years before other symptoms appear. Unlike acne, once the disease begins it becomes progressive and self-perpetuating. Extensive, deep, dermal inflammation results in large, painful abscesses. The healing process permanently alters the dermis. Cordlike bands of scar tissue criss-cross the axillae and groin. Reepithelialization leads to meandering, epithelial-lined sinus tracts in which foreign material and bacteria become trapped. A sinus tract may be small and misinterpreted as a cystic lesion. The course varies among individuals from an occasional cyst in the axillae to diffuse abscess formation in the inguinal region.
Like acne, the plugged structure dilates, ruptures, becomes infected, and progresses to abscess formation, draining, and fistulous tracts. In the chronic state, secondary bacterial infection probably is a major cause of exacerbations.
Management:
Tretinoin cream (0.05%) may prevent duct occlusion, but it is irritating and must be used only as tolerated. Large cysts should be incised and drained, whereas smaller cysts respond to intralesional injections of triamcinolone acetonide (Kenalog, 2.5 to 10 mg/ml). Weight loss helps to reduce activity.
Antibiotics are the mainstay of treatment, especially for the early stages of the disease. As with acne vulgaris, long-term oral antibiotics such as tetracycline (1 gm daily), erythromycin (1 gm daily), or minocycline (200 mg daily) may prevent disease activation. High dosages, such as 500 mg of erythromycin four times daily for an average-sized adult, are effective for active disease.
Isotretinoin (1 mg/kg/day for 20 weeks) may be effective in selected cases. The response is variable and unpredictable and complete suppression or prolonged remission is uncommon.
Surgical excision is at times the only solution. Residual lesions, particularly indolent sinus tracts, are a source of recurrent inflammation. Local excision is often followed by recurrence. Wide excision of affected skin, and healing by granulation or applying split skin grafts or transposed or pedicle flaps, affords better control. Local recurrence after wide excision varies greatly with the disease site.
REF: Habif: Clinical Dermatology, 3rd ed., 1996
IMPETIGO (See Bacterial Infections)
The three key possibilities are tinea cruris (fungus), intertrigo (hot, sweaty, irritated skin) and erythrasma (a bacterial infection/colonization).
Avoid strong topical steroids (Class I and II) and combination steroids (e.g. Lotrisone®, Mycolog®) in the groin.
Treatment
Perform KOH if available.
OTC Zeasorb AF® is helpful for hot, sweaty irritated skin.
Try an anti-fungal for 2 weeks. If the patient has already tried Clotrimazole Cream, use Lamasil® Cream, OTC or Spectazole (Econazole®) Cream.
If there is no improvement, add Hydrocoritsone or Desonide (Desowen®) 1% or 2% Cream. If no improvement, refer to Dermatology
ITCHING ALL OVER,
LITTLE OR NO RASH
![]()
![]()
Consider
Dry skin (See Dry Skin.)
Scabies (See Scabies.)
Endocrinologic conditions (thyroid disease, diabetes mellitus)
Neoplastic disease
Drugs (prescribed, recreational, herbal)
Other conditions (hepatitis, iron deficiency anemia)
Lichenification means increased skin markings. Look for a thickened plaque in a typical area such as the dorsal foot, scrotum/vulva, or extremity. The condition is usually asymmetric.
Do not be afraid to tell the patient, "don't scratch! It does not matter how strong a steroid I give you, if you continue scratching, you will continue to have the rash."
Treatment
For the groin: Betamethasone Valerate (Valisone®) 0.1% cream BID for 2 weeks maximum
For involvement elsewhere: Betamethasone Diproprionate (Diprolene®) 0.05% ointment BID for 3 weeks is recommended.
Consider antihistamines.
If there is no response to treatment after 3-4 weeks, refer patient to Dermatology.
Pediculus humanus var capitis, corporis, pubis (crabs)
Pubic lice, or crabs, is seen the most common.
Signs: excoriation, infection, adenopahty.
Diagnosis: nits (What you need to do is look closely at the hair,
particularly at the roots of the hair, at the base of the scalp and over
the ears.)
Treatment
For the scalp & body & pubic lice :
Permethrin 1% cream rinse for 5-10 min (OTC- Nix ®) should be used.
Advise patient to apply to the scalp for 5-10 minutes then rinse. The treatment
should be applied to dry hair for optimum efficacy. Successful treatment
usually requires removing the nits as well as many will not be affected.
They may be combed out with a fine-toothed comb after pretreatment with a
loosening agent (OTC "Step 2"®).
Lindane 1% shampoo for 5-10 min
* Retreat symptomatic patients in 1 week.
It is important to remove lice and their nits from the hair DAILY with a metal comb. Combs, brushes, hats, etc. must also be treated. The permethrin should be reused in 7-10 days. It is important to examine and if needed treat all members in a family. Inform school and other close contacts.
For the groin:
Permethrin rinse 1% (OTC -Nix®) Applying rinse from the trunk
to knees is sufficient.
Cysts Images
Keloids Images Acne keloidalis
Lipomas
Pyogenic Granuloma Images
Venous Lake Images
Dermatofibroma Images
Treatment
Recognize and refer appropriate, symptomatic patients.
It is more common in women than in men.
Most commonly appears as symmetric brown patches on the face of a woman, frequently noted during pregnancy or while on hormone therapy (e.g. BCPs, HRT). However, it may occur with out a specific cause.
Treatment
Hydroquinone 3-4% (e.g. Solaquin Forte® gel/cream or Melanex® solution) applied to dark areas BID with or without Avita® 0.025% cream QHS for a minimum of 6 months. Not all patients will respond. Advise daily morning SPF 30 sunscreen.
Molluscum is caused by a virus. Although it commonly affects children, adults may be affected as well. It may be sexually transmitted in adults.
Molluscum appears as multiple skin-colored to pink papules. There may be only a few or there may be more than 50. They may be grouped or scattered. Often the surrounding skin is irritated and red.
Treatment
Liquid nitrogen (cryotherapy) or curettage may be performed on individual lesions. For numerous lesions, e.g., in beard or groin areas: Apply Retin A® 0.05% Cream once daily for several months until resolved.
Nummular eczema presents as very itchy, round or oval, eczematous areas. Occurs in the setting of dry skin.
Treatment
Limit daily shower to 5-minutes. Use cold or warm water and mild, non-perfumed, non-dyed cleansers, e.g., Dove® unscented soap. Avoid long, hot showers.
Therapy requires a relatively high-potency (Class II topical steroid Betamethasone Dipropionate (Diprolene®) 0.05% or Fluocinolone (Lidex®) 0.05% ointment. Apply Betamethasone Diproprionate (Diprolene®) ointment to red, inflamed areas immediately after the shower and cover the rest of the skin with Cetaphil® or Eucerin® cream, Aquaphor®, SBR-Lipocream® or petrolatum. No lotions please. If the condition worsens with topical steroids, rethink the diagnosis. Could it be tinea? See atopic dermatitis for additional treatment recommendations.
REF: fungal_nail2009.pdf
A culture should be performed before initiating oral therapy.
Check a CBC and SGPT (ALT) at baseline and after one month.
Recommended treatment for fingernails:
Onycymycosis of the fingernails is a covered benefit. Terbinafine
(Lamasil®) 250 mg QD for 6 weeks
Recommended treatment for toenails:
Onychomycosis of the toenails is only covered for diabetics and patients
presenting with functional symptoms. Remember that 1 out of 3 older patients
with thickened, abnormal nails does not have fungus.
Terbinafine (Lamasil®) 250 mg QD for 12 weeks.
Topical antifungal agents, e.g. Loprox® Lotion may be helpful for mild or superficial onychomycosis.
The patient must wait a year for full results and use an OTC topical antifungal (Clotrimazole or Terbinafine) agent long term to prevent recurrence.
Advise patients to keep the nails trimmed.
Peri-oral Dermatitis
REF: Dr.
Arndt's Dermatology in Primary Care 2002 Kenneth Arndt,
MD
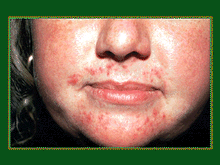
It looks like rosacea, but it's not, and this is an important diagnosis, because it's common, seen almost only in women. Red bumps around the mouth, so it's perioral, and you have the area immediately around the vermilion border spared, so this is perioral dermatitis, something that didn't exist when I was a resident but certainly exists and is common now, seen only in women in their 20's and 30's, cause unclear. It's seen in young women, may last a long time; it certainly can be seen as a side effect of the use of topical steroids on the face, but in most cases the cause is not clear.
Red papules and pustules: sometimes it's red behind it, may be scaly. It can be seen; some people call it periorificial, because you can see a little bit around the nose and sometimes a little around the eyes, and it usually has some symptoms, a little burning and stinging, not too much itching.
Therapy of Perioral Dermatitis:
Topical: stop steroids, start metronidazole gel/cream bid
If necesssary, oral antibiotics: tetracycline, doxycycline, or minocycline
Options: low potency steroid,as hydrocortisone, desonide, alclometason; topical or oral erythromycin
Well, you stop anything that may be turning it on - steroids - and you use usually topical metronidazole, which in 60 - 80% of cases, within six weeks you get it under pretty good control. It makes the inflammatory part go away or get much better; it makes the flushing and blushing a little bit better. If that isn't sufficient, use a systemic antibiotic, and if it's quite inflammatory, you can use a very low potency - i.e., hydrocortisone cream, hydrocortisone, desonide, which is another low-potency steroid. You can use topical antibiotics, but usually metronidazole is the best of the bunch.
Many patients experience an initial larger lesion (herald patch) 1-2 weeks before the eruption. Characteristic lesions include round or oval plaques with scale at the periphery. The rash has a predilection for the sun-protected sites of the trunk, axilla, groin and neck and may or may not be itchy.
[Pityriasis Rosea REF: Dr. Arndt's Dermatology in Primary Care 2002 -
Fir-tree scaling plaques
Herald spots: 50-90%
Pruritus:50%
Duration: 2-10- weeks
No sequela; "immunity" in 98%
Seen equally in men & women; most patients aged 10-43; increased in spring & fall
Etiology unknown - ? infection, hypersensitivity, immunologic.
Treatment:
Usual: topical antipruritics (such as calamine, Sarna, PramaGel, Pramoxine,
Zonalon; Aveeno baths, topical corticosteroids), sun, lubricants
Severe: topical, systemic corticosteroid as Prednisone; Ultraviolet B
phototherapy. ]
Treatment
Rule out secondary syphilis with RPR.
For localized itching: Triamcinolone acetonide (Kenalog®) 0.1% cream/ointment BID as needed until symptoms abate. For widespread itching: Hydrocortisone 2 1/2% Lotion BID as needed until itching subsides. Tell patient rash may persist for 1-3 months.
Characteristic lesions include red, scaly plaques on the elbows and knees. Scalp involvement is common as well. A Strep or other infection may precipitate a flare.
[Scaling plaques on extensors, scalp
Asymptomatic or pruritic/painful
Nail pitting, onycholysis, dystrophy
Alternative forms: guttate, pustular, erythrodermic, arthritis
Early onset = greater severitiy
Genetically determined, hyperproliferative
Lithium, beta blockers, steroid withdrawal exacerbate
Therapy:
Topical corticosteroids (as Temovate/Ultravate/Diprolene ointment
initially), potent, alone or with occlusion
Intralesional corticosteroids (triamcinolone 3-5 mg/ml)
Systemic steroids: AVOID if possible
Calcipotriene (Dovonex) ointment, cream, solution, vitamin D3. Use
bid, < 100g/week may be an irritant
Tazorac (tazarotone) gel 0.05 - 0.1% - new topical retinoid,
use with topical steroids
For Extensive Psoriasis Rx:
UVB phototherapy; Psoralen phototherapy; Methotrexate; Systemic retinoids
(etretinate as Soriatane); Cyclosporin 3 - 5 mg/kg
Treatment
Excellent control, but not cure is the realistic goal of therapy.
For the scalp:
Shampoo at least 2-3 times/week with T/gel®, T/sal®, selenium sulfide
(Selsun®) 2.5% shampoo (RX needed), Baker's P&S® shampoo etc.
For non- responsive areas:
Add Fluocinonide (Lidex®) 0.05% or Clobetasol (Temovate®) solution
to scalp QD-BID as needed. May reduce to Fluocinolone acetonide (Synalar®)
0.01% for maintenance. May shampoo in-between with non-medicated shampoos
as desired. Note that African American patients should not shampoo more than
every 5-7 days.
For elbows, knees and body:
Betamethasone Diproprionate 0.05% (Diprosone®) ointment BID.
Many patients improve with sunlight. Psoriasis requires high potency topical steroids unless it is on the face or on areas in body folds. When the psoriasis improves, consider less frequent application of current treatment or a lower potency topical steroid for maintenance.
Advise patients that excess alcohol consumption, tobacco and certain medications (e.g. beta-blockers or lithium) may precipitate or flare psoriasis.
Refer patients with greater than 10% body involvement to Dermatology.
ROSACEA
![]()
![]() See also
Rosacea
See also
Rosacea
Characteristic lesions include symmetrically distributed papules and pustules on the nose and cheeks. Telangiectasias and flushing are commonly associated findings but they do not respond to medical therapy. (Patients may have laser therapy for facial telangiectasias; however this is not a covered benefit and will and will only be treated for a fee.)
It is kind of a sebaceous, thick skin, a little bit swarthy, but this is with a lot of acneiform lesions so there are a lot of papules and pustules, no blackheads. So if you're not sure it's acne or if it's rosacea: rosacea you get no blackheads, no comedones; you just get pustules, sometimes cysts. It's in the middle third of the face, so it's on the cheeks, it's on the chin but it's not laterally. The nose is a little big here, so you can get sebaceous hyperplasia of the nose, going on to rhinophyma in men.
Flushing & Blushing: preRosacea
Erythroma & telangiectasia
Inflammatory papules/pustules
Rhinophyma (it can now be treated nicely with carbon dioxide laser therapy)
Ocular signs & symptoms: conjunctivitis, blepharitis, keratitis
Differential Dx of Rosacea:
SLE, Acne vulgaris, Perioral dermatitis, Seborrheic dermatitis, Cutaneous
sarcoid, Cutaneous TB, Leprosy
Treatment of Rosacea:
Avoid trigger factors, which are the flushing and blushing; the people are much more sensitive usually to heat, exercise-induced heat, alcohol-induced heat, drug-induced heat, emotions
Redness: green-tint cover up; clonidine 0.05 mg 1-2/d; laser therapy
Inflammatory: metronidazole gel/cream as Metrogel or Metrocream; clindamycin lotion; oral antibiotics as tetracycline, doxycycline, minocycline, erythromycin
Rhinophyma: laser surgery
Treatment:
Tetracycline 500 mg BID for 3-4 weeks then taper to lowest effective dose, e.g. one pill QD or one QOD.
Topical Metrogel or cream (Metronidazole)
apply bid , or
Sulfur and Sodium Sulfacetamide (Sulfacet®, Novacet®)
is a helpful adjunct but is not as effective as Tetracycline.
Finacea (Acelaic acid) 15% gel for the topical Rx of the inflammatory papules & pustules of mild to moderate rosacea.
SCABIES
![]()
![]() See also
Scabies
See also
Scabies
So this is infestation with a mite, and mites by definition
pretty much are just small enough you can't see them with the naked eye,
and this typically is a disease in which the itching is worse at night. Now
all itching is worse at night. Anything that itches: when you go to bed,
you stop moving around, you stop having other things on your mind, your body
heats up a bit - it's going to itch worse. Scabies, however, itches really
bad at night. You see it often in certain areas: hands, genitalia, in body
folds, sometimes in the popliteal fossa. It may resemble a bunch of things:
exzema, impetigo, dermatitis, psoriasis, and so forth; typically, burrows
on interdigital area, nodules on genitalia.
When you get infected, it doesn't itch, and the itching is actually from
sensitization to the mite, so it's one to three months from the time
you get exposed and infested to the point you begin to itch, and the spread
is like with lice: it can be person-to-person, but often it is just someone
in the same bed as or sharing clothing or towels with. The mites don't travel
much, and once they drop off of someone, they don't live a long time, a few
days.
1-3 months from exposure to lesions
If untreated, can persist indefinitely
Spread: person to person, formites, prolonged exposure
Mites do't travel much, short viability of host (3-5 days)
Diagnosis: scrape burrows for mites or feces (scybala)
Look for burrows (thread-like scaly) in the wrists, web spaces and sides of feet. Inflammatory papules on the penis are classic for scabies.
Symptoms:
The lesions may be red or appear as white, gray, or black thread-like lines.
The lesions can be intensely pruritic, especialy at night.
Occasionally 2-5 mm nodules appear or vesicles develop, esp. in children.
The lesions can get secondarily infected with Streptococcus pyogenes
or Staphylococcus aureus.
Diagnosis:
Definitive diagnosis of scabies is made by recovering the mite from a burrow
by skin scraping & looking at the skin scraping under a microscope.
Sensitivity of this method is low in typical scabies but very high in crusted
scabies.
Treatment
Elimite® (Permethrin) 5%
cream for 8-12 hours is the drug of choice: Prescribe
enough medication to treat the immediate family (60 grams is sufficient to
treat 2 adults). Apply cream from the neck down and leave on overnight. In
AM, shower. Apply to scalp in anyone with scalp itching. Do not shower prior
to applying medication.
A large study compared 5% permethrin cream with 1% lindane lotion.
Complete resolution occurred in 91% of patients treated with permethrin and
in 86% of patients given lindane. Pruritis persisted in 14% of the permethrin
group and in 25% of the lindane group. Permethrin is safe and effective.
One application is highly effective for treating scabies and is a safe
alternative to lindane.
Wash all bedding and clothing in warm or hot water and then dry in the dryer. Cloth items, which cannot be laundered or dry-cleaned, may be bagged and stored for 7-10 days.
Oral Stromectol (Ivermectin) is also effective for crusted scabies, although not approved for this purpose by the FDA.
Oral antihistamines & topical steroids may be used for the itching.
* Family members must be treated at he same time, & a good environmental cleaning of the home is essential.
133.0B SCABIES
- will treat with Stromectol (ivermectin) 200 mcg/kg PO as 18 mg (Six 3 mg tablets). Repeat dose in 1-2 weeks.
- prednisone 20 mg daily x 10 days for severe itching and inflammation
- Elimite® (permethrin) 5% cream to spouse over night
- wash bedding and PJ's on hot cycle
* Kwell® 1% (Lindane = gamma benzene hexachloride) cream, shampoo, and lotion. - is no longer available for sale in California. ? Some dermatologists feel that the cream is the most reliable form of medication for scabies.
REPORTING
Reporting of single cases of atypical or crusted scabies & outbreaks
of scabies are mandated & should be reported immediately by telephone
to the Communicable Disease Reporting System Hotline at (888) 397-3993
SEBORRHEIC
DERMATITIS
![]()
![]() seborrheic_dermatitis2009.pdf
seborrheic_dermatitis2009.pdf
Characteristic lesions include redness and scaling along the nasolabial fold, eyebrows, and scalp. Severe cases may affect much of the face.
[Dandruff is not seborrheic dermatitis, but it kind of merges with it, so seborrheic dermatitis - there are more red, delimited plaques rather than diffuse, but they are both proliferative disorders: eyebrows, scaling in the eyebrows, scaling in the nasolabial folds, which is very common, or behind the ears.
Erythema, scaling on scalp, brow, nasolabial, postauricular areas
Mustache, beard, chest too
May have blepharoconjunctivitis
Pruritus of scalp is universal
In HIV disease more severe, recalcitrant
Onset: puberty to adult years
More common in men than women
Cause: correlated with sebaceous gland activity
Yeast Pityrosporum ovale has critical role (so if you use something that affects these yeasts, such as some topical antifungals, itraconazole for instance, it gets better. So topical ketoconazole, Nizoral, is therapy which has been shown to be helpful.)
Therapy of Seborrheic Dermatitis:
Shampoos: ketoconazole (Nizoral), selenium sulfide (Selsun), zinc
pyrithione 5-10 min qd x 10-14d
Corticosteroid solutions for itch, scaling: betamethasone (Valisone),
fluocinonide (Lidex)
Low/medium strength steroids for body, cheeks
Topical ketoconazole
Options: short hair/beard; chloroxine (Capitrol); Blephamide Liquifilm
for blepharitis
Treatment
Excellent control, not cure is the realistic goal of therapy.
Use medicated shampoo to lather scalp and face as often as daily initially, leave on 5-10 minutes then taper as possible, but use forever.
Recommended Shampoos include: OTC: Nizoral® 1% shampoo, Head and Shoulders®, T/gel®, T/sal®.
Consider prescription Rx for failure of OTC products: Selenium sulfide 2%
For the face:
Hydrocortisone 1% cream may be applied daily for persistent redness and scale.
An alternative for facial seborrheic dermatitis is Ketaconazole (Nizoral®)
1% cream QD-BID.
For itching of the scalp:
Use a liquid steroid, e.g. Fluocinolone acetonide (Synalar®) 0.01% solution.
May be used QD after shampooing with a medicated shampoo.
The goal is to recognize patients who have suspected skin cancers. Patients with suspected skin cancers should then be referred to Dermatology for further evaluation and treatment.
Basal cell carcinomas (BCCs)
are usually pearly, translucent papules (nodular type) or flat, ham-colored
red areas (superficial type). However, they may be pigmented.
Squamous cell carcinomas (SCCs)
classically are hyperkeratotic, growing papules or nodules.
Keratoacanthomas
classically are rapidly growing nodules with a central keratotic
core.
Melanoma Images
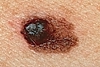 Asymmetry
Asymmetry
 Border
Border
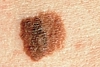 Color
Color
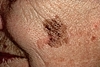 Diameter
>6 mm
Diameter
>6 mm
usually appears as asymmetric, irregularly bordered pigmented lesions with
varied colors. Characteristic lesions are frequently > 6mm as well as
smaller lesions that are undergoing change.
All of these occur in the chronically sun exposed areas. Superficial BCCs are common on the back and legs.
Refer suspected BCCs, SCCs, keratoacanthomas and melanomas to Dermatology.
Stasis dermatitis presents as an eczematous eruption that occurs on the lower legs in some patients with venous insufficiency. It mot commonly affects the lower 2/3 of the legs and frequently involves the area surrounding the inner ankle.
Skin in the affected area appears red and scaly. Edema is always present and may be severe. Varicosities may be seen about the lower leg. An ankle flare may be present. Over time, the skin may take on a brownish discoloration due to residual hemosiderin. In severe cases, ulceration may occur.
Treatment
Edema must be controlled primarily by wearing support hose. The patient is often resistant to wearing support hose; however, it is critical to educate the patient that treating the edema with the use of support hose is essential to the care of this condition. Patients should be instructed to put support hose on as early as possible in the morning and to remove them just before going to bed.
In order to control the eczematous changes, a medium potency topical steroid, e.g. tramincinolone acetonide (Kenalog®) 0.1% ointment may be given.
Additional supportive measures include: diuretic therapy for edema, limiting sodium intake, avoiding standing for long periods of time, and elevating the legs.
Skin Fungal Infections /
TINEA
PEDIS -
![]()
![]() &
Images
of Tinea Infections
&
Images
of Tinea Infections
Clinical presentations may vary. Initially appears as red, scaly, macerated areas in the web spaces. Then, the scale spreads to the sole. In the fully developed stage, the entire sole is involved in a "moccasin" distribution.
[Dematophytes - well marginated, red, annular patch, central clearing
May itch, sting
Types classified by anatomic location: tinea pedis (athlete's foot), cruris (jock itch), corporis (body), nail (onychomycosis), manus
T. Corpus
In the groin fungal infection, you have to look at the feet, because the
way these hyphae get there, almost always, is people who have chronic fungal
infection of the feet, and then it gets carried up on a towel or whatever,
so if you just treat the groin, and you don't look at the feet, then the
groin will clear up but it will get reinfected, so you really do have to
look elsewhere.
Therapy of Skin Fungal Infection:
OTC cream: clotrimazole, miconazole
Spectazole/ econazole; Lamasil/ terbinafine; Loprox/ cicloprox cream or lotion
bid for 4 weeks
Compresses of exudative & aeration if macerated
Oral: Lamisil (Terbinafine) 250 mg qd x 6 wks for fingernails &
12 wks for toenails; Pulse Sporonox (Itraconazole) 200 mg bid
first wk of the month for 3 months
When you are using it for 12 weeks, it is suggested that you get liver function
tests before and at six weeks.]
Tinea pedis - Start terbinafine cream BID (after soaking/washing when time permits then apply hydrocortisone 1% ointment generously for up to 1 month until clear & smooth.
Look for onychomycosis as well.
Treatment
OTC: Clotrimazole (Lotrimin AF®), Miconazole (Micatin®) or Terbinafine (Lamisil®) Use BID to entire foot for at least 2 weeks. Zeasorb AF® (an OTC powder) can be put in shoes or shaken into socks daily.
Rx: Spectazole (Econazole®) Use QD-BID for at least 2 weeks.
If not responsive to treatment, consider foot eczema.
TINEA VERSICOLOR
Lesions classically occur on the oily areas of the trunk of a young adult. The areas may be hypo- or hyperpigmented or pink. Scratching the area shows a fine scale.
[Slightly scaling macules, dark or light, primarily on truck
Usually asymptomatic
Non-contagious, relapsing fungal infection Malassezia furfur, Pityrosporum
ovale, Pityrosporum orbiculare
More in summer, tropical climates
Adolescents, young adults: 1% in US, up to 50% in tropics
Predisposing: humidity, hyperhydrosis, BCP, pragnancy, steroids, immunosuppresion
Covert saprophytic yeast to mycelial or hyphal form
Depigmentation develops: tyrosinase inhibited by dicarboxylic acids produced by M. furfur
Biopsy: scraping; "spaghetti & meatballs"
Therapy of Tinea Versicolor:
Shampoos: selenium 2.5% (Selsun), zinc pyrithione 1.0 - 2.5% for 5-10 min
for 2 wks, then once q 2-4 wks
Tropical antifungals cream or lotion: bid x 2-3wks
PO Ketoconazole 400 mg or 200 mg/d x 5 days
Fluconazole 400 mg dose once
Itraconazole 200 mg/d x 7d
Griseofulvin is not effective ]
Treatment
KOH shows a spaghetti and meatball pattern of the fungus Pityrosporum.
Selenium Sulfide (Selsun®) 2.5% shampoo; taper to Selenium Sulfide 1%. Lather trunk for 10 minutes QD for 7 days, then taper to once every 2 weeks for prophylaxis. Clotrimazole 1% cream may be applied BID to localized areas. Let patients know that it may take 1-2 months for skin color to return to normal.
Acute Urticaria
If the urticaria has been present for less than 6 weeks it is considered acute urticaria. Typically acute urticaria lasts a few days to a few weeks. There are no routine laboratory studies for the evaluation of acute urticaria. Ask about possible precipitating factors including food and drink, medications, e.g. aspirin, change of environment, recent travel, exposure to pollen or chemicals.
Most cases present with typical urticarial plaques (hives) larger than 2 cm. Stroke the patient's arm to rule out dermatographism.
Most urticaria is self-limited.
Treatment
Treatment is directed toward symptomatic relief and the use of antihistamines, e.g. Diphenhydramine hydrochloride (Benadryl®) 25-50 mg q6h, Hydroxyzine (Atarax®) 10-25 mg q6h, Doxepin Hydrochloride (Sinequan®) 10-25 mg tid, Fexofenadine (Allegra) 60 mg bid or Loratadine (Claritin) 10 mg 1/day. Sedating antihistamines are best used at bedtime and non-sedating antihistamines in the morning.
If the patient presents with evidence of throat involvement, treatment is more aggressive with the use of epinephrine subcutaneously, steroids (IV initially, orally later), and EpiPen®) for future emergency use.
If there is purpura, or the lesions stay in the same spot over 24 hours, refer to Dermatology (may represent urticarial vasculitis).
[The drug of choice for control of urticaria is an H1 antihistaminic. In difficult cases, a combination of H1 and H2 antihistamines (as Tagemet-Cimetidine 300 mg q6h) may be more effective. Also, doxepin (Sinequan 10-25 mg tid) has both H1 and H2 antihistaminic properties and can be used when a single H1 agent fails to control disease activity. Severe or refractory urticaria may benefit from a prednisone 40-60 mg taper in combination with an antihistamine agent.- EMedicine Nov.2001]
Chronic Urticaria
Patients who have a history of hives lasting for 6 or more weeks are classified as having chronic urticaria. The etiology is often unclear.
Treatment
If patient has chronic urticaria over 6 weeks, refer to Allergy for evaluation.
VITILIGO
![]()
![]() REF:
Vitiligo
2009
REF:
Vitiligo
2009
Vitiligo is a condition in which the skin loses its color in well-defined patches. They usually start small and expand. The extremities and the face are commonly involved. Patients 10-30 years of age are most commonly affected. Patients over 40 years of age who develop what appears to be new onset vitiligo should have a complete skin examination to rule out melanoma
Vitiligo occurs in about 1-2% of the population. A family history is present about 20-30% of the time and is more commonly seen in patients with younger onset of disease. It seems to represent an autoimmune condition in which the patient's own immune system is attacking the pigment-producing cells. Various autoimmune conditions (e.g. thyroid disease, pernicious anemia) are sometimes associated with vitiligo; however frequency is not high enough to warrant routine screening for vitiligo.
Treatment
There is no uniformly effective treatment for vitiligo. This is unfortunate as it can be psychologically devastating, especially in those patients with darker skin. Health care providers should be sensitive to the patient's emotional state.
Camouflage may be helpful for lesions on the face, hands, and other exposed areas. Various department stores with extensive cosmetics, e.g., Dermablend®, may be a good resource. Protection from the sun is important to prevent photodamage. Various skin dyes (e.g. self- tanners, vitadye) are available, but the color match is often less than optimum and overlap at the edges can make for uneven pigmentation.
Remember that treatment is not uniformly successful nor is it required. Refer patients to Dermatology for evaluation and treatment as appropriate. Treatment may include the use of topical steroids for a period of 2-4 months. Caution must be taken to assure that atrophy does not occur. Another option is systemic PUVA therapy for a 6 month period of time.
If on the sole, be sure to confirm the diagnosis by paring. A wart has black dots; a corn has a clear center.
Treatment
For plantar warts: Home topical treatment can be very effective. Mediplast 40% daily or cryotherapy. Cryotherapy treatments can be performed as frequently as every 2-3 weeks. Use two applications of liquid nitrogen at each treatment session. Freeze wart until it turns white with a 1 mm margin. Repeat one time after thawing. Encourage home care between cryotherapy treatments. OTC salicylic acid QD (same ingredient as in medicated corn pads, e.g. Mediplast which has 40% salicylic acid) and paring every 2-3 days is a helpful adjunct to cryotherapy.
For other warts: One application of liquid nitrogen as described above at each clinic visit. Home support is helpful and should include topical salicylic acid preparations, e.g. Compound W.
Condyloma Acuminatum
Treatment: (CDC 1998)
Patient Applied
Podofilox
(Condylox) 0.5% solution or gel (3.5 mL)
Apply to the wart(s) two times a day for three days in a row for
up to 4 weeks using an applicator tip or finger. Skip four days by not applying
any medicine for four days in a row. If the wart can still be seen, this
application cycle may be repeated each week for up to four weeks, until the
wart is gone.
or
Imiquimod 5% cream
(Aldara)
Apply a thin film to wart once every other day (three times a week) before
normal sleeping hours. Rub in well and leave on for six to ten hours. Remove
medicine from wart by washing with mild soap and water. Continue treatment
until wart is gone or for up to sixteen weeks.
Provider Administered
Cryotherapy or
Podophyllin resin 10%-25% in tincture of benzoin (Podofin
or Podocon-25)
Apply to the affected area(s) of the skin and leave on the skin
for one to six hours. Treatment may be repeated every week for up to six
weeks.
or
Trichloroacetic acid
(TCA)
or Bichloroacetic acid (BCA) 80%- 90% or
Surgical removal
XEROTIC ECZEMA (See Dry Skin.)
Potency of
Drugs
![]()
![]() REF:
Topical_steroids2009.pdf
REF:
Topical_steroids2009.pdf
I - Psoriasis (except body folds), allergic contact dermatitis, most rashes of the palms and soles, nummular eczema, pompholyx, lichen Simplex Chronicus
Clobetasol (Temovate, Cormax)
Betamethasone diproprionate, augmented (Diprolene) 0.05% ointment
II -
Betamethasone diproprionate (Diprosone) 0.05% ointment
Fluocinonide (Lidex) 0.05%
Flurandrenolide (Cordran Tape )
III - Asteatotic or other severe eczemas
Betamethasone dipropionate (Diprosone) 0.05% cream
Betamethasone valerate (Valisone) 0.1% ointment
IV - Adult eczema, resistant childhood eczema
Fluocinolone acetonide (Synalar) 0.035% ointment
Triamcinolone (Kenalog) 0.1% ointment
V - Resistant facial rashes, childhood eczema
Betamethasone valerate (Valisone) 0.1% cream or lotion
Fluocinolone acetonide (Synalar) 0.025% cream
Triamcinolone acetonide (Kenalog) 0.1% cream or lotion; 0.025% ointment
VI - Resistant facial rashes, childhood eczema
Betamethasone valerate (Valisone) 0.01% cream
Desonide 0.05% cream, ointment, lotion
Fluocinolone acetonide (Synalar) 0.01% cream or solution
Triamcinolone acetonide (Kenalog) 0.025% cream or lotion; 0.025% ointment
VII - Seborrheic dermatitis of face, infantile eczema of face, most dermatitis of the face
Hydrocortisone OTC 1% or 2.5% cream, lotion, or ointment
Benign Skin Conditions (Considered Cosmetic)
Please note:
Visits or procedures for the following conditions are not covered benefits and are performed on a fee for service basis where available, unless otherwise stated.
ANDROGENETIC ALOPECIA
Androgenetic alopecia is not a covered benefit. Look for the pattern of hair loss. Hair loss on the top of the scalp is usually androgenetic.
BRUISES ON THE ARMS (Bateman's, Senile or Solar Purpura)
Many adults bruise very easily on the arms after the slightest trauma or even after no trauma at all. This occurs because sun damage has made the elastic tissue of the superficial blood vessels brittle and no longer pliable. This allows leakage of red blood cells out of the vessel with minimal provocation. The bruise tends to fade over a month or two. Steroid use can thin the skin and make this worse. Sun exposure also adds to the thinning.
CAPILLARY HEMANGIOMAS Images of Hemangiomas
Most adults over 30 have one or more red vascular papules on the trunk. They are little dome-shaped or slightly raised papules. In one study of adults 30-39 years of age, 90% of the men and 65% of the women had at least one cherry hemangioma. There seems to be no good reason to have these, but luckily, they are not dangerous. There is no home remedy for capillary hemangiomas. If the patient desires, they can be removed by a cosmetic dermatologist.
Many women will complain of this bump on the leg. It may be pink, red, tan, or brown. The key distinguishing feature is that you can grab it between two fingers and feel it within the dermis. Often, when you do this, the surface will be "sucked in". The upper back, especially over the scapula is another typical area. Men may also be affected. The surface of the dermatofibroma is often pigmented, and at times, velvety. There is no home remedy for dermatofibromas. If the patient desires, they can be removed by a cosmetic dermatologist.
DERMATOSIS PAPULOSA NIGRA
DPN is a common papular condition of the face and neck in darker-skinned patients. They appear as multiple, brown, papules, small plaques and pedunculated lesions occur on the
face neck and upper trunk in a darker-skinned patient. No treatment is needed. If the patient desires, cosmetic removal may be pursued.
EPIDERMAL INCLUSION CYST
The epidermal inclusion cyst--formerly known as the sebaceous cyst--is a sphere of skin within the skin. The cyst wall constantly flakes into the center of the cyst causing it to enlarge over time. A central pore is usually visible. Often the lesion periodically drains, releasing a foul smelling white material. At other times, the lesion may become acutely inflamed. This is usually a result of rupture of the cyst wall and release of the cyst contents into the surrounding dermis. A foreign body response results. Asymptomatic epidermal inclusion cysts do not need to be treated. If however, one large enough to be bothersome or if it periodically gets inflamed, it may be removed surgically. This is a covered benefit.
If the lesion becomes acutely inflamed, apply warm compresses twice a day. Such an inflammatory episode may actually cause to cyst to go away. If not, the lesion may be surgically excised after the inflammation has subsided. Surgery acutely will be very difficult with much intraoperative bleeding and pain.
FRECKLES
Freckles are caused by the sun. Light-skinned, red-haired patients are most susceptible. They appear as light tan or brown spots scattered on the face or nose of a child or young adult. The patient and/or parents should be educated on sun avoidance, sunscreens, and skin cancer.
LENTIGINES
Lentigines are flat, brown spots appearing on aged exposed skin, frequently on the back of the hands. They are due to the accumulation of lipofuscin in the tissue as one ages. They are commonly referred to as "liver spots"; however, there is no physiological relationship to the liver.
MILIA
These tiny, white bumps on the face are most common in women. They represent tiny, benign cysts. There is no home remedy for milia, although over time, they may work themselves out. If the patient desires, they can be removed by a cosmetic dermatologist.
SEBACEOUS HYPERPLASIA
This 3 mm. "yellow donut" is a common inhabitant of the face of an older adult. The characteristic 2-4 mm donut shape is classic and the yellowish color confirms the suspicion. This lesion requires no therapy. If the patient desires, they can be removed by a cosmetic dermatologist.
SEBORRHEIC KERATOSES Seborrheic Keratosis images
Most acommon benign tumor; it's scaly, it's warty, and indeed it's warty because it's verrucous
Found in adults > 45 years old
May be inflamed, painful, pruritic or asymptomatic
Can mimic melanoma, basal cell carcinoma
Therapy: They can be ignored because they are benign, but they can be symptomatic or cosmetically a problem. They can be treated with liquid nitrogen, cryotherapy, curettage, scrape them off, electrosurgery, and there are no topical agents that are effective.
This "barnacle" on the ship of life can take on so many different appearances. It may be brown, black, white or tan, dry and warty or smooth and greasy. They are most common on the trunk, but may occur anywhere. As to why people get them, there is no good answer. They are very common, and are not dangerous or contagious. They often run in families. There is no home remedy for seborrheic keratoses. If the patient desires, they can be removed by a cosmetic dermatologist.
These tabs are common in the armpit, on the neck, in the groin and under the woman's breasts. They catch on necklaces, rub on collars and bras etc. Skin tags serve no good purpose. They seem to arise in areas of friction and they are slightly more common in taller patients and those of increased weight. For the majority their presence is another mystery of life. There is no home remedy for skin tags. If they are symptomatic, those lesions can be removed as a covered benefit. If not symptomatic and the patient desires, they can be removed by a cosmetic dermatologist.
SYRINGOMA
The syringoma is a benign growth that most commonly occurs below the eyes. They are a little more common in women of Asian descent and they may run in families. They appear as multiple flesh-colored papules on the lower eyelids and upper cheek. No treatment is necessary. Cosmetic surgery may be pursued.
TELANGIECTASIAS
Telangiectasias commonly occur on the face and legs of middle-aged and older adults. Telangiectasias appear as small, thread-like blood vessels visible just below the skin's surface. On the face, the nose and cheeks are the most commonly affected areas, and the patient is usually fair-skinned. Facial telangiectasias may occur in association with rosacea, but they may not. Indeed, a patient with facial telangiectasias without pimples or pustules does not have rosacea. It must be emphasized that tetracycline and other medications for rosacea do not remove facial telangiectasias. Telangiectasias do not require treatment. If the patient prefers, cosmetic laser surgery may be done.
Telangiectasias of the legs (or spider veins) are common as well. No treatment is needed. Wearing support hose can decrease the development of future telangiectasias. If the patient desires, they may be seen and treated by a cosmetic dermatologist or plastic surgeon for sclerotherapy or other cosmetic (non-covered) treatment.
WRINKLES
Treating wrinkles is not a covered benefit. If the patient desires, wrinkles can be treated by a cosmetic dermatologist.
XANTHELASMA
Xanthelasma are soft, yellow deposits about the eyes. They appear as soft, yellow plaques on the upper inner eyelids although they can occur below the eyes as well. They may occur
as an isolated finding or associated with elevated lipids and/or cholesterol. All patients with xanthelasma should have a lipid profile. No treatment is needed although cosmetic surgery may be pursued.
Poison Ivy or Oak Contact Dermatitis
- secondary to Urushiol irritation
Rx: Zanfel solution wash
Skin Ulcer Care | Wound Rx 2008.pdf
By: Rolf Paulson, MD, Pat Guthmiller, RN, BSN CWOCN, Dan Rustvang, RN, MSN,
FNP-C
Source: Patient Care November 1, 2005
ROLF PAULSON, MD, Medical Director, Chronic Wound Care Clinic, Altru Clinic and Hospital; Clinical Professor of Internal Medicine, University of North Dakota School of Medicine and Health Sciences, Grand Forks, ND.
The diagnosis and treatment of chronic wounds has received inadequate attention in medical schools and primary care residencies. Attention to wound management, especially the care of chronic cutaneous ulcers, is generally scattered throughout medical and surgical specialties, rehabilitation medicine, podiatry, dermatology, and primary care.
We have a 4-step protocol currently in use at our institution for the management of chronic cutaneous ulcers.
The first and most important step is to determine and address the cause
of the wound.
Edema secondary to venous valvular incompetence, for example, can
cause stasis ulcers; diabetes is a frequent cause of neuropathic ulcers;
and arterial insufficiency often causes ulcers that lead to gangrene.
The next step is to evaluate any comorbidities that may interfere with wound healing, such as arterial insufficiency that is preventing resolution of a heel ulcer caused by immobility, infection that is complicating healing of a statis ulcer, or neuropathy, arterial insufficiency, and infection all complicating healing of a ulcer.
Third, we evaluate how well the patient understands the nature of the ulcer and the healing process, their motivation to improve, and the need for resources, such as caregivers, money or insurance for dressings or equipment, and transportation. A positive outlook and healing environment will optimize the outcome.
The fourth and last step is to evaluate the wound and determine the appropriate treatment, type of dressing needed, and the need for debridement.
History and physical examination
At our institution, patients with chronic ulcers undergo a thorough history taking, physical examination, and, when appropriate, special studies. A complete history puts the wound in context; a history of arterial or venous disease or vasculitis is particularly important in the patient with a nonhealing leg ulcer. How was the initial wound treated? What treatments for previous ulcers have been successful? Has the patient undergone skin grafts or vascular bypass? What caused immobility that led to the decubitus ulcers? Does the patient appear well nourished?
During the wound examination, note the appearance of the wound itself and the surrounding skin and the presence and absence of pulses, edema, and other clues to the underlying cause. Measure the wound and note any necrosis, slough, or granulation tissue. Probe any fissures or deep aspects to the wound. Document the size and composition of the wound, including granulation tissue, eschar, or slough with both a flow chart and a digital camera. Images are excellent documentation for both the clinical staff and the patient; many patients with sacral or heel ulcers have never seen their wound.
A clinical suspicion of inadequate arterial supply that is suggested by the ankle-brachial ratio warrants formal arterial Doppler flow studies. Laboratory studies including serum albumin level, WBC count, and ESR may give evidence of inflammation and the patient's nutritional status. A suspicion of osteomyelitis warrants consideration of a bone scan or MRI. A biopsy may be in order if the history and examination are inconclusive regarding the type of ulcer.
Treatment
Ulcer treatment occurs in 2 phases;
first, the ulcer is prepared for healing, and then healing is promoted (see "Treating specific ulcers").
Because healing will not occur until granulation tissue has formed, the first step is to debride necrotic tissue or slough. Sharp debridement using a scalpel or scissors to remove necrotic tissue can be performed in the operating room or in the office. Mechanical debridement involves the use of a whirlpool, abrasive treatment, or wet-to-dry dressings to mechanically remove debris. Enzymatic debridement requires the use of a topical agent such as collagenase to remove and dissolve the slough. Autolytic debridement, or moist wound healing, involves the use of hydrocolloids, transparent films, and hydrogels to enable the body's own enzymes to eliminate devitalized tissue and encourage growth of granulation tissue. Advantages of autolytic debridement include less pain, less frequent dressing changes, and faster healing. Moist wound healing consists of occluding the wound, keeping the surface moist, keeping the edges dry, and removing exudate.
TABLE 1. Dressings for ulcer care
Among the many available dressings, those used most commonly for ulcer treatment fall into either moisture-retentive or drying agents. Made of nonwoven fibers derived from seaweed, alginate dressings form an absorbent gel on contact with wound exudate. They are typically used for wounds with moderate to heavy drainage. Hydrocolloid dressings are composed of gelatin and gel-forming agents such as sodium carboxymethylcellulose. They also form an absorbent gel on contact with exudate and are used for wounds with light to moderate drainage. Hydrogel dressings contain a gel composed primarily of water and are used for wounds with minimal or no exudate (see Table 1). Wounds with extreme exudate may benefit from the use of vacuum-assisted closure.
SUGGESTED READING
Baranoski S, Ayello E. Wound Care Essentials: Practice Principles. Philadelphia, Pa: Lippincott Williams & Wilkins; 2004.
Boulton AJ, Kirsner RS, Vileikyte L. Clinical practice: neuropathic diabetic foot ulcers. N Engl J Med. 2004;351:48-55.
de Araujo T, Valencia I, Federman DG, et al. Managing the patient with venous ulcers. Ann Intern Med. 2003;138:326-334.
Lyder CH. Pressure ulcer prevention and management. JAMA. 2003;289: 223-226.
Sumpio BE. Foot ulcers. N Engl J Med. 2000;343:787-793.
Takahashi PY, Kiemele LJ, Jones JP Jr. Wound care for elderly patients: advances and clinical applications for practicing physicians. Mayo Clin Proc. 2004;79:260-267.
Treating specific ulcers
IMAGES: ROLF PAULSON, MD
Stasis ulcers
The appearance of stasis ulcers, the most common type of chronic ulcer, is typically one of a shallow, irregularly shaped wound that is often hyperpigmented and usually occurs on the medial or lateral malleolus. Effective management of the constant edema is the key to treatment. At our institution, treatment using a 4-layer compression bandage system is often successful; patients tolerate the 4-layer compression bandages much better than they do the Unna boot dressings.
A wound dressing can be used under the 4-layer bandage. The initial 4-layer dressing is usually changed after 3 or 4 days and then weekly thereafter. Compression should only be initiated with adequate circulation. Stockings typically exert 30 to 40 mm of compression, although a greater degree of compression is often used in obese patients. We have found that antiembolism stockings provide inadequate compression in a wound care setting.
Healing a stasis ulcer is often easier than keeping it healed. Patients must understand the consequences of discontinuing compression.
Arterial ulcers These often painful ulcers caused by arterial insufficiency can occur anywhere, but appear most often in the feet. Gangrene of the toes or foot is a worrisome presentation of arterial insufficiency. Treatment is aimed at restoring blood flow, and options include revascularization by surgery or angioplasty. Amputation is a last resort.
Diabetic foot ulcers
These painless neurotrophic or neuropathic ulcers typically occur on the plantar surface of the foot below the first metatarsal head, at the heel, or at the top of the toes. Treatment involves eliminating the pressure that caused the ulcer and addressing any arterial deficiencies or infection; the latter can be complex and require complicated antibiotic regimens. Osteomyelitis is assessed by exam, x-ray studies, bone scan, or MRI and treated appropriately with antibiotics, surgery, or both.
Decubitus ulcers
The crucial element of treating these ulcers is relieving the pressure, or offloading. As for heel or other pressure ulcers, observe the patient in both the sitting and supine positions in the chair or mattress used regularly to determine the best way to alleviate pressure. The appropriate dressing depends on staging (see Table 1). In stage 1 decubitus ulcers, the skin is unbroken but red or otherwise discolored that does not fade within 30 minutes of the pressure being relieved. Stage 2 ulcers are characterized by a torn or broken top layer of skin that creates a shallow, open wound. Stage 3 ulcers are deeper than stage 2, and the wound extends through the fatty tissue. Stage 4 ulcers extend into the muscle and necrotic tissue, and drainage is often noted.
CLINICAL PEARLS
Examine dressings removed from wound, and note type and consistency of exudate.
Limit or modify use of adhesive dressings on fragile skin.
The silver-based dressings are antimicrobial and are appropriate for methicillin-resistant Staphylococcus aureus wounds.
Ischemic pain is extremely difficult to control. If pain is controlled and surgery is considered too risky, observation is a reasonable approach, with the understanding that thewound will not heal. Uncontrolled pain or infection warrants urgent revascularization or amputation.
Debridement is not an emergency, and the clinical situation may worsen when the patient with inadequate circulation undergoes debridement.
Get help! As difficult as it is to be mindful of the available dressings, it is more difficult to have them available and have the right reimbursement codes at the ready. Teaming with an RN or certified wound ostomy care nurse (CWOCN) works very well in our chronic wound care setting.
OTC Mederma gel
Scarless gel (from Plastic Surgery Clinic)
Table of Contents | Drugs | Med News & Journals | Guidelines & Textbooks | Diff-Dx | Resource | |
|
ACP Medicine | ACP Online | Annals | PIER | Epocrates |