Claudication | Peripheral Arterial Vascular Disease (PVD) See Claudication 2007
![]() TOC |
Cardiology
TOC |
Cardiology
![]()
Claudication |
Peripheral Arterial Vascular Disease (PVD)
See
Claudication 2007
Medical Treatment of Peripheral Arterial Disease
(Evaluated by a resting ankle-brachial systolic BP index of <
0.90)
- JAMA, Feb. 1, 2006 - Vol 295: 547 Graema J Hankey,
etc.
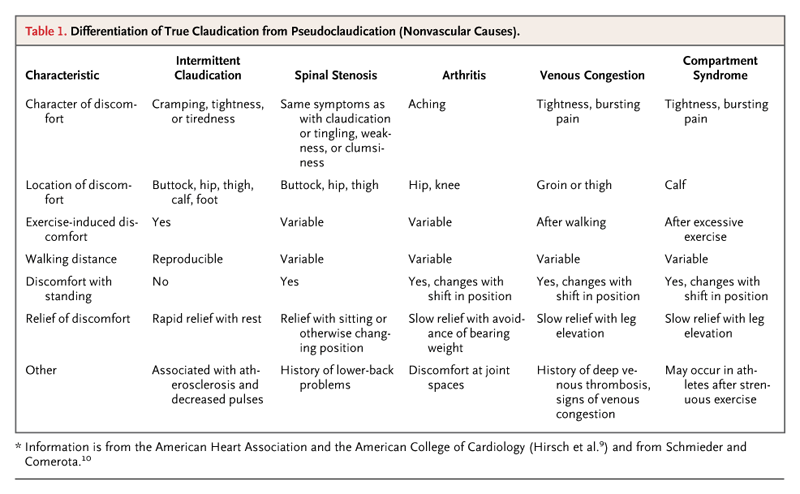
Differential Diagnosis of Claudication
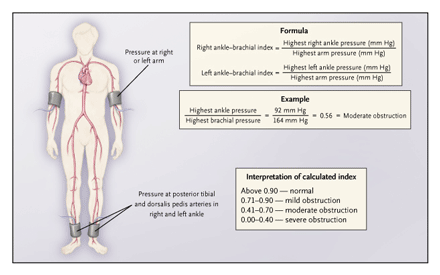
Pressure Measurement
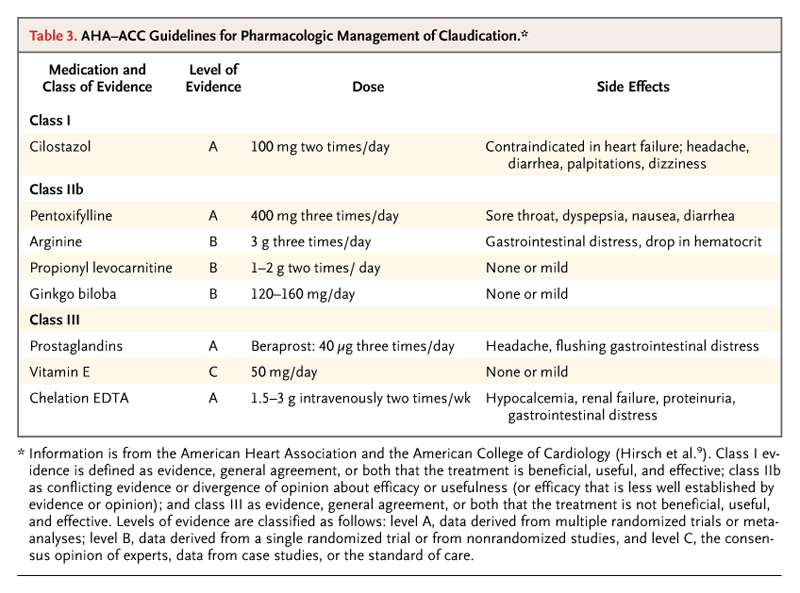
Drug Rx for Claudication
Cilostazol (Pletal) 50-100 mg
Bid Useful in Treating Intermittent Claudication
Arch
Intern Med September 27, 1999;159: 2041-2050 - Hugh Beebe,
etc.
Dawson DL - Circulation - 1998 Aug 18; 98(7): 678-86
The platelet aggregation inhibitor cilostazol improves pain-free and maximal walking distances in patients with intermittent claudication. The only possible drug-related side effects (headache, abnormal stool or diarrhea, dizziness, palpitations) all resolved without treatment. These data demonstrate the safety and effectiveness of cilostazol in treating intermittent claudication.
Ticlopidine (Ticlid) Reports from Europe (level II) have shown a beneficial effect of ticlopidine for relieving symptoms, increasing walking distance, and improving lower-extremity ankle pressure indexes. [19] [20] In addition, a meta-analysis of these trials has demonstrated that patients with intermittent claudication treated with ticlopidine had a significant reduction in fatal and nonfatal cardiovascular events in comparison with patients treated with placebo. [21] In a multicenter, randomized clinical trial, use of ticlopidine (250 mg/d) in patients with claudication was shown to result in a need for fewer vascular surgery procedures over a 7-year period than use of a placebo control. [22] The need for subsequent vascular surgery was reduced by about half (relative risk, 0.486; p < 0.001). The specific indications for the subsequent vascular procedures were not addressed, nor was the risk of adverse events such as neutropenia. Ticlopidine is associated with adverse hematologic effects generally not associated with aspirin. In addition to neutropenia, thrombotic thrombocytopenic purpura has recently been reported in 60 patients taking ticlopidine. [23] Although promising, there is a need for confirmatory studies before ticlopidine can be recommended.
Pentoxifylline, has been reported to improve abnormal erythrocyte deformability, reduce blood viscosity, and decrease platelet reactivity and plasma hypercoagulability. Thus, pentoxifylline is a weak antithrombotic agent and its beneficial effects may stem from other pharmacologic properties. A number of clinical trials (levels I and II) have evaluated pentoxifylline. Many concluded that pentoxifylline was significantly more effective than placebo in improving treadmill walking distances, but six trials could not demonstrate consistent benefit. In most trials, patients treated with placebo also had significant improvement and this tended to obscure benefits attributable to active drug treatment. A critical review of these trials concluded that the actual improvement in walking distance attributable to pentoxifylline is often unpredictable, may not be clinically important compared to the effects of placebo, and does not justify the added expense for most patients. The drug may have a role in a few patients with markedly reduced walking distances who are unresponsive to or cannot engage in exercise therapy; for such patients, even a small increase in claudication walking distance may allow activities that were previously impossible.
Intermittent Claudication Revisited: The Value of Medical Therapy - William
R. Hiatt
(Arch
of IM Sep.13, 1999:159 No.16)
2006