THYROIDITIS |
REF: NEJM Volume 348:2646-2655 June 26, 2003
|
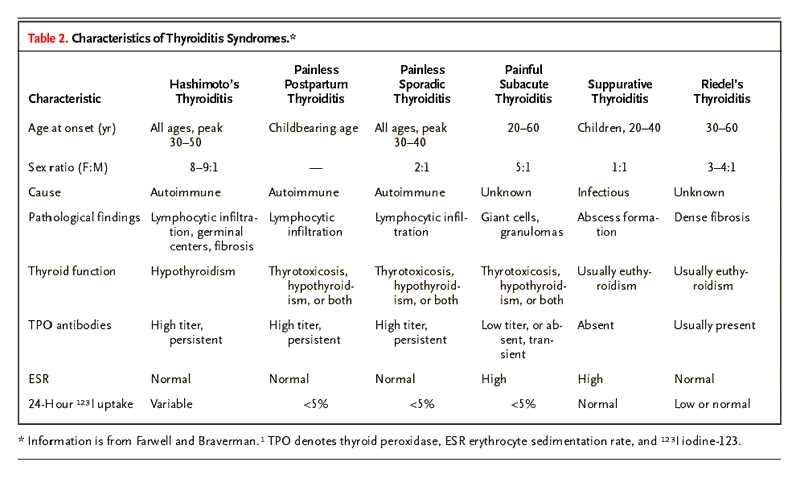
Types of Thyroiditis (Terminology
for Thyroiditis)
-
Hashimoto's thyroiditis
(Chronic lymphocytic thyroiditis, Chronic autoimmune thyroiditis, Lymphadenoid
goiter)
- TPO (Thyroid peroxidase) antibodies: high titer, persistent; ESR:
Normal; RAIU: variable
-
Painless postpartum thyroiditis
(Postpartum thyroiditis, Subacute lymphocytic thyroiditis)
- TPO antibodies: high titer, persistent; ESR: Normal; RAIU: <5%
-
Painless sporadic thyroiditis
(Silent sporadic thyroiditis, Subacute lymphocytic thyroiditis)
- TPO antibodies: high titer, persistent; ESR: Normal; RAIU: <5%
-
Painful subacute thyroiditis
(Subacute thyroiditis, de Quervain's thyroiditis, Giant-cell thyroiditis,
Subacute granulomatous thyroiditis, Pseudogranulomatous thyroiditis)
- TPO antibodies: low titer, or absent, transient; ESR: high; RAIU:
<5%
-
Suppurative thyroiditis -
The disease may prove fatal if
diagnosis and treatment are delayed.
(Infectious thyroiditis, Acute suppurative thyroiditis, Pyrogenic thyroiditis,
Bacterial thyroiditis)
- TPO antibodies: absent; ESR: high; RAIU: Normal
-
Drug-induced thyroiditis
(amiodarone, lithium, interferon alfa, interleukin-2)
-
Riedel's thyroiditis
(Fibrous thyroiditis)
- TPO antibodies: usually present; ESR: Normal; RAIU: low or normal
Hashimoto's thyroiditis, painless sporadic thyroiditis, and painless postpartum
thyroiditis all have an autoimmune basis.
 |
 |
| Hashimoto's
Thyroiditis
-
The most common type of thyroiditis
-
The most frequent cause of hypothyroidism and goiter,
in an occasional patient, hyperthyroidism alternates with hypothyroidism,
most likely owing to the intermittent presence of thyroid-stimulating and
thyroid-blocking antibodies.
-
It is characterized by the presence of high serum thyroid antibody
concentrations and goiter.
-
EXAM: A firm, bumpy, symmetric,
painless goiter is frequently the initial finding
About 10 percent of patients with chronic autoimmune hypothyroidism
have atrophic thyroid glands (rather than goiter), which may represent
the final stage of thyroid failure in Hashimoto's thyroiditis.
-
TESTS:
- High serum thyroid peroxidase antibody concentrations are present
in 90% of these patients.
- High serum thyroglobulin antibody concentrations are present in
20-50% of these patients.
- The thyroid appears hypoechogenic on ultrasound examination.
- The 24-hour radioactive iodine RAIU (iodine-123) uptake is not
helpful in establishing the diagnosis.
-
RX: Once overt hypothyroidism or
subclinical hypothyroidism (with high serum thyroid antibody concentrations)
is present, levothyroxine sodium is the treatment of choice.
The goal of replacement therapy with levothyroxine sodium is
normalization of serum thyrotropin values.
In patients with Hashimoto's thyroiditis and a large goiter,
thyrotropin-suppressing doses of levothyroxine sodium can be
given over the short term (i.e., six months) to decrease the
size of the goiter. In most patients with Hashimoto's thyroiditis
(whether their condition is euthyroid or hypothyroid), goiter
size will decrease by 30 percent after six months of therapy
with levothyroxine sodium. Replacement doses should be resumed
if the size of the goiter does not decrease. Because serum
thyroid antibody concentrations do not decrease with levothyroxine
sodium therapy, except in some patients with hypothyroidism,
monitoring of these concentrations is not indicated once the
diagnosis of Hashimoto's thyroiditis has been made.
Although thyroid lymphoma is very rare, the risk of this disease is
increased by a factor of 67 in patients with Hashimoto's
thyroiditis. Patients with Hashimoto's thyroiditis and a dominant
thyroid nodule should undergo fine-needle aspiration biopsy
to rule out lymphoma and thyroid carcinoma. When thyroid carcinoma
occurs in patients with this type of thyroiditis or other
lymphocytic infiltration, the prognosis appears to be more favorable
than when it does not.
 |
|
| Painless
Postpartum Thyroiditis
-
It occurs within the first few months after delivery. It
occurs in up to 10 percent of women in the United States.
-
It is most common in women who have
- high serum thyroid peroxidase antibody concentrations during
the first trimester of pregnancy or immediately after delivery
- other autoimmune disorders, such as type 1 diabetes mellitus,
or with a family history of autoimmune thyroid disease.
-
CLINICAL COURSE:
Thyrotoxicosis typically begins one to six months after
delivery and lasts for one to two months.
That phase may be followed by a hypothyroid phase starting
four to eight months after delivery and lasting four to six
months.
Clinical course may show thyrotoxicosis during the first three months, followed
by hypothyroidism for three months and then by euthyroidism.
Eighty percent of women recover normal thyroid function within
a year;
in one follow-up study, however, permanent hypothyroidism
developed within seven years in 50 percent of the women studied.
After a first episode of painless postpartum thyroiditis, there is a 70%
chance of recurrence with subsequent pregnancies.
Chronic hypothyroidism is more likely in multiparous women or
in those with a history of spontaneous abortion.
-
EXAM: In most cases a small,
nontender, firm goiter is present.
-
TESTS:
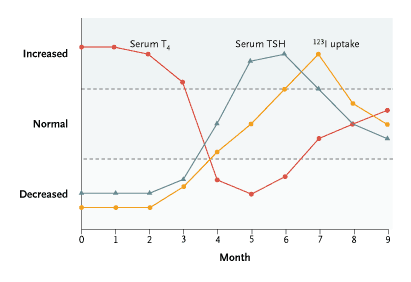
- in only 1/3 of patients will the classic triphasic thyroid hormone pattern
develop (Figure 2)
- High serum concentrations of thyroid peroxidase antibodies,
thyroglobulin antibodies, or both, are also present.
- The erythrocyte sedimentation rate is normal.
- The 24-hour 123I uptake (RAIU) is low (<5%), distinguishing it
from postpartum Graves' disease whereas it is elevated.
This test should be performed in patients with symptomatic thyrotoxicosis
when there are no clear signs of Graves' disease, such as large
goiter or ophthalmopathy.
Because radioactive iodine is secreted in breast milk and
123I has a half-life of 13 hours, nursing mothers need
to pump and discard milk for at least two days after the test.
-
RX: Mild thyrotoxicosis rarely
requires therapy, but when the disease is severe, it is treated
with beta-blockers.
Antithyroid drug therapy is contraindicated, because
there is no excess thyroid hormone production.
Treatment of the hypothyroid phase may not be necessary, but if
this phase is prolonged or if the patient is symptomatic,
levothyroxine sodium should be given, then withdrawn after six
to nine months to determine whether thyroid function has
normalized.
 |
|
| Painless
Sporadic Thyroiditis
-
Painless postpartum thyroiditis and painless sporadic
thyroiditis are indistinguishable except by the relation of the
former to pregnancy.
-
It may represent a subacute form of Hashimoto's thyroiditis.
-
It may account for about 1 percent of all cases of thyrotoxicosis.
-
The clinical course is similar to that of painless postpartum
thyroiditis. Although abnormalities in thyroid function resolve
in most patients, 20 percent of patients will have residual
chronic hypothyroidism. Overall recurrence rates have
not been well established.
-
Symptoms are usually mild.
-
EXAM: A small,
nontender, very firm, diffuse goiter is present in 50
percent of these patients.
-
TESTS:
- High serum thyroid peroxidase antibody concentrations
are present in 50 percent of patients at the time of diagnosis,
with lower titers, on average, than in Hashimoto's
thyroiditis.
- The 24-hour 123I uptake (RAIU) is low (<5%) can be diagnostic,
and the test should be performed when the cause of the thyrotoxicosis
is unclear, in order to avoid inappropriate treatment with antithyroid
drugs.
-
RX: Therapy is the same
as that for painless postpartum thyroiditis.
 |
|
| Painful
Subacute Thyroiditis
-
It is a self-limited inflammatory disorder, is the most
common cause of thyroid pain.
-
It occurs in up to 5 percent of patients with clinical thyroid
disease.
-
It frequently follows an upper respiratory tract infection, and
its incidence is highest in summer, correlating with the peak
incidence of enterovirus.
A viral cause of subacute thyroiditis has therefore been proposed,
but so far clear evidence for it is lacking.
-
SX:
- Subacute thyroiditis begins with a prodrome of generalized myalgias,
pharyngitis, low-grade fever, and fatigue.
- Patients then present with fever and severe neck pain,
swelling, or both.
- Up to 50 percent of patients have symptoms of thyrotoxicosis.
-
CLINICAL COURSE:
In most patients, thyroid function will be normal after several
weeks of thyrotoxicosis, and hypothyroidism will subsequently
develop, lasting four to six months, as in painless sporadic
thyroiditis and painless postpartum thyroiditis. Although thyroid
function normalizes spontaneously in 95 percent of patients over
a period of 6 to 12 months, residual hypothyroidism persists
in 5 percent of patients. Painful subacute thyroiditis recurs
in only about 2 percent of patients.
-
TESTS:
- A markedly elevated erythrocyte sedimentation rate is
the hall mark of painful subacute thyroiditis
- The C-reactive protein concentration is similarly
elevated. - The leukocyte count is normal or slightly
elevated.
- Elevated Free T4 and T3, with ratios of T4 to T3
of greater than 20, reflecting the proportions of stored hormone
within the thyroid, and
- Serum concentrations of thyrotropin TSH are low or
undetectable.
- Serum thyroid peroxidase antibody concentrations are usually
normal.
- The 24-hour 123I uptake is low (<5%) in the
toxic phase of subacute thyroiditis, distinguishing this disease
from Graves' disease.
Color-flow Doppler ultrasonography may also help to make
this distinction; in patients with Graves' disease the thyroid
gland is hypervascular, whereas in patients with painful subacute
thyroiditis the gland is hypoechogenic and has low-to-normal
vascularity.
-
RX:
The treatment for painful subacute thyroiditis is to provide
symptomatic relief only.
Nonsteroidal medications or salicylates are adequate to control
mild thyroid pain.
For more severe thyroid pain, high doses of glucocorticoids
(e.g., 40 mg of prednisone daily) provide immediate relief;
doses should be tapered over a period of four to six weeks.
Corticosteroids should be discontinued when the 123I
uptake returns to normal.
Beta-blockade controls the symptoms of thyrotoxicosis.
Therapy with levothyroxine sodium is rarely required, because
the hypothyroid phase is generally mild and transient,
but it is indicated for symptomatic patients.
 |
|
| Suppurative
Thyroiditis
-
It is rare
-
Suppurative thyroiditis is usually caused by bacterial infection,
but fungal, mycobacterial, or parasitic infections may also
occur as the cause.
-
It is most likely to occur in patients with preexisting thyroid
disease (thyroid cancer, Hashimoto's thyroiditis, or multinodular
goiter), those with congenital anomalies such as a pyriform sinus
fistula (the most common source of infection in children), and
those who are immunosuppressed (as HIV, AIDS), elderly, or
debilitated.
-
SX & EXAM: usually
acutely ill with fever, dysphagia, dysphonia, anterior neck
pain and erythema, and a tender thyroid mass.
Symptoms may be preceded by an acute upper respiratory infection.
The presentation of fungal infection, parasitic infection,
mycobacterial thyroiditis, and opportunistic thyroid infection
in patients with AIDS tends to be chronic and insidious.
-
TESTS:
- Thyroid function is generally normal in patients with suppurative
thyroiditis, but both thyrotoxicosis and hypothyroidism have
been reported.
- Leukocyte counts and erythrocyte sedimentation rates are
elevated.
- Suppurative areas appear "cold" on radioactive-iodine
scanning.
- Fine-needle aspiration biopsy with Gram's staining and
culture is the diagnostic test of choice.
-
RX: The therapy for
suppurative thyroiditis consists of appropriate antibiotics
and drainage of any abscess.
The disease may prove fatal if diagnosis and treatment are
delayed.
 |
|
| Drug-Induced
Thyroiditis
Many medications can alter thyroid function or the results of
thyroid-function tests. However, only a few are known to provoke
autoimmune or destructive inflammatory thyroiditis.
Amiodarone
Amiodarone-induced hypothyroidism
occurs in up to 20 percent of patients in iodine-sufficient regions.
Patients with preexisting thyroid autoimmunity are at increased
risk for the development of hypothyroidism while receiving
amiodarone.
Amiodarone-induced thyrotoxicosis
occurs in up to 23 percent of patients receiving amiodarone and
is far more prevalent in iodine-deficient regions.
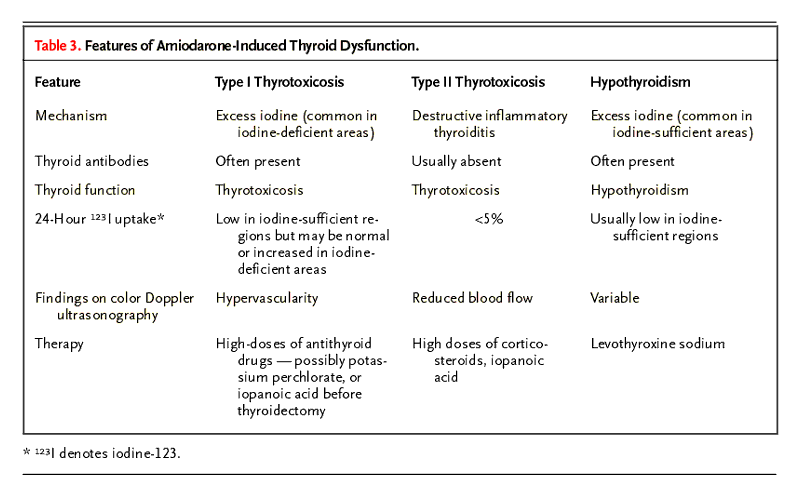
Two Types of Amiodarone-induced Thyrotoxicosis
-
Type I amiodarone-induced thyrotoxicosis is defined as
synthesis and release of excessive thyroid hormone; it is
iodine-induced,
and it is more likely to occur in patients with preexisting
subclinical thyroid disorders, especially nodular goiter.
RX: It is best treated with high doses of antithyroid
drugs (methimazole/Tapazole or propylthiouracil/PTU), sometimes with
the addition of potassium perchlorate to prevent further uptake of iodine
by the thyroid.
- Lithium has also been suggested as therapy for type I disease.
- Iopanoic acid has recently been reported to be effective in
patients with type I disease who require
thyroidectomy.
-
Type II amiodarone-induced thyrotoxicosis is a destructive
thyroiditis that causes the release of preformed thyroid hormone
from the damaged thyroid gland.
RX: It responds to high-dose corticosteroids.
- Iopanoic acid has recently been reported to be effective in
patients with type II amiodarone-induced thyrotoxicosis, although
less so than corticosteroids.
Distinguishing between the two forms of amiodarone-induced
thyrotoxicosis is difficult, especially since some patients have
both types.
Although the serum interleukin-6 concentration was initially reported to
be more elevated in type II amiodarone-induced thyrotoxicosis than in type
I, subsequent studies have not replicated this finding.
TESTS:
-
In patients in the United States, 123I uptake values
are typically low in type I and type II amiodarone-induced
thyrotoxicosis.
-
Color-flow Doppler ultrasonography may show hypervascularity in
type I disease but reduced blood flow in type II.
-
Careful examination of the thyroid, base-line thyroid-function
tests, and measurements of serum concentrations of thyroid
peroxidase and thyroglobulin antibodies should be performed before
amiodarone therapy is instituted, and thyroid function should
be monitored every six months as long as patients are receiving
the drug.
RX: Treatment with levothyroxine
sodium is indicated in hypothyroid patients, and amiodarone may
be continued. The dose of levothyroxine sodium needed to
normalize the serum concentration of thyrotropin is often higher
than the usual dose, because amiodarone decreases 5'-deiodinase
activity in peripheral tissues, thus also decreasing production
of T3.
Lithium
-
In patients with preexisting thyroid autoimmunitiy, lithium may increase
the serum thyroid antibody concentrations and lead to subclincal or overt
hypothyroidism.
-
Estimates of the prevalence of high serum thyroid antibody concentrations
in patients receiving long-term treatment with lithium range from 10-33%.
-
In addition, thyrotoxicosis has been reported after long-term
lithium use, possibly caused by lithium's direct toxic effects
on thyroid cells or by lithium-induced painless sporadic thyroiditis.

Interferon Alfa and
Interleukin-2
Thyroid-function tests and measurements of serum thyroid antibodies
should be performed before therapy with interferon alfa or
interleukin-2 is initiated and every six months thereafter.
In up to 15% of patients during interferon alfa therapy may develop
-
high serum thyroid peroxidase antibody concentrations or
-
thyroid dysfunction
Interferon alfa has also been reported to cause destructive
inflammatory thyroiditis.
High serum thyroid peroxidase antibody concentrations in such
patients and in patients receiving interleukin-2 therapy
may be associated with
-
overt or subclinical hyperthyroidism (Graves' disease)
or
-
hypothyroidism
The measurement of 123I uptake RAIU helps to distinguish
between
-
drug-induced Graves' disease, in which the uptake is
elevated, and
-
drug-induced inflammatory thyroiditis, in which the uptake
is low, in patients with thyrotoxicosis.
RX:
-
When Graves' disease develops in patients receiving interferon alfa
therapy, they should be treated with antithyroid drugs.
While treatment with interferon alfa or interleukin-2 is continued
-
The thyrotoxic phase of inflammatory thyroiditis can be treated
with beta-blockers and, if necessary, with nonsteroidal
antiinflammatory drugs or corticosteroids
-
The hypothyroidism can be treated with levothyroxine sodium.
Although thyroid function usually normalizes when cytokine therapy
is discontinued, affected patients are at increased risk for
autoimmune thyroid dysfunction in the future.
 |
|
| Riedel's
Thyroiditis (Fibrous thyroiditis)
-
Riedel's thyroiditis, a local manifestation of a systemic fibrotic
process, is a progressive fibrosis of the thyroid gland that
may extend to surrounding tissues.
-
The prevalence of this disease is only 0.05 percent among patients
with thyroid disease requiring surgery, and its cause is unknown.
-
SX: symptoms due to tracheal
or esophageal compression or hypoparathyroidism due to extension
of the fibrosis into adjacent parathyroid tissue.
-
Most patients are euthyroid at presentation but become
hypothyroid once replacement of normal thyroid tissue is nearly
complete.
-
EXAM: a rock-hard,
fixed, painless goiter.
-
TESTS: High serum thyroid
antibody concentrations are present in up to 67 percent of
patients, but it is unclear whether the antibodies are a cause
or effect of the fibrotic thyroid destruction.
-
DX: A definitive diagnosis
is made by open biopsy.
-
RX: The treatment is surgical,
although therapy with glucocorticoids, methotrexate, and tamoxifen
has been reported to be successful in the early stages of the
disease.
 |
|
|
Among patients with Hashimoto's thyroiditis, hypothyroidism is more likely
to develop in smokers than in nonsmokers. An increased prevalence of
painless postpartum thyroiditis has also been noted among smokers.
In addition, geographic variations in the incidence of Hashimoto's
thyroiditis, painless postpartum thyroiditis, and painless sporadic
thyroiditis suggest that dietary iodine insufficiency may
be protective against autoimmune thyroiditis.
Clinical Course of Painful Subacute Thyroiditis, Painless Postpartum Thyroiditis,
and Painless Sporadic Thyroiditis.
Measurements of serum thyrotropin (TSH) and iodine-123 (123I)
uptake show thyrotoxicosis during the first three months, followed by
hypothyroidism for three months and then by euthyroidism. T4 denotes
thyroxine.